"Cheap clarinex 5mg, allergy testing one year old".
By: E. Alima, M.B. B.CH. B.A.O., M.B.B.Ch., Ph.D.
Co-Director, Rutgers New Jersey Medical School
Dexamethasone is usually given only on days 1-4 in even-numbered cycles because of toxicity allergy forecast montreal quebec 5mg clarinex mastercard. Methylprednisolone allergy testing kits buy cheap clarinex 5mg on-line, 2 g three times weekly intravenously for a minimum of 4 weeks allergy medicine blood thinner cheap 5 mg clarinex mastercard, is helpful for patients with pancytopenia and may have fewer side effects than from dexamethasone allergy forecast east lansing discount clarinex 5mg visa. The use of interferon as a single agent for these patients has been disappointing. The reversal of resistance to chemotherapeutic agents is an important area of research. The use of verapamil or quinine to reverse the resistance to doxorubicin has been disappointing. Hypercalcemia, present in 15 to 20% of patients at diagnosis, should be suspected in the presence of anorexia, nausea, vomiting, polyuria, polydipsia, increased constipation, weakness, confusion, or stupor. Hydration, preferably with isotonic saline plus prednisone (25 mg four times per day), relieves the hypercalcemia in most cases. The dosage of prednisone must be reduced and its use discontinued as soon as possible. If these measures fail, bisphosphonates such as pamidronate disodium or etidronate disodium are beneficial. Patients with myeloma should be encouraged to be as active as possible because prolonged bed rest contributes to hypercalcemia. This complication occurs in half of patients with multiple myeloma and may develop insidiously or rapidly (acute renal failure). Plasmapheresis may be helpful for regaining renal function, but patients with severe myeloma cast formation or other irreversible changes are unlikely to benefit from plasmapheresis. Maintenance of a high urine output (3 L/day) is important for preventing renal failure in patients with Bence Jones proteinuria. Prophylactic penicillin often benefits patients with recurrent gram-positive infections. Fixation of fractures or impending fractures of long bones with an intramedullary rod and methyl methacrylate has produced good results. Patients in a prospective study receiving 90 mg of pamidronate every 4 weeks had fewer skeletal complications and improved quality of life; this medication is recommended for myeloma patients with skeletal involvement. Hyperviscosity is usually manifested by oronasal bleeding, blurred vision, or heart failure. Serum viscosity levels do not correlate well with the symptoms or clinical findings. Plasmapheresis promptly relieves the symptoms and should be done regardless of the viscosity level, if the patient is symptomatic. Spinal cord compression from an extramedullary plasmacytoma should be suspected in patients with severe back pain, the development of weakness or paresthesias of the lower extremities, or bladder or bowel dysfunction. Prognosis Multiple myeloma has a progressive course, and the median survival is approximately 3 years. The bone marrow plasma cell labeling index and beta2 -microglobulin level are the most important prognostic factors in previously untreated multiple myeloma. Cytogenetics contribute important and independent prognostic information: partial or complete deletion of chromosome 13, chromosome 11q abnormalities, and the presence of any translocation are predictors of a poor outcome. Patients who respond rapidly to chemotherapy and who have an increased plasma cell labeling index have a shorter remission and survival. Twenty to 30 per cent of patients survive 5 or more years, but fewer than 5% survive longer than 10 years. In some patients, an acute or aggressive terminal phase is characterized by rapid tumor growth, pancytopenia, soft tissue subcutaneous masses, decreased M-protein levels, and fever; the survival in this subset is usually only a few months. Often, a small amount of M-protein is found in the urine and the concentration of normal immunoglobulins in the serum is decreased. These patients must be observed over time because symptomatic multiple myeloma develops in many of them.
Syndromes
- Coma
- Preschooler test or procedure preparation (3 to 6 years)
- Lupus nephritis
- Infants younger than 12 months can usually eat formula, cereal, or baby food until about 6 hours before surgery. They may have clear fluids and breast milk until 4 hours before surgery.
- Green and red peppers
- Side effects of medications
- Worked with sheet metal in the past (you may need tests to check for metal pieces in your eyes)
- Feeding difficulties
- Tests to detect or rule out certain birth defects (such as Down syndrome)
- It is severe
Fatty acid oxidation is inhibited allergy shots effectiveness buy 5mg clarinex fast delivery, and there is a corresponding decrease in adenosine triphosphate production and gluconeogenesis allergy testing health partners order clarinex 5mg on-line. Continuing fatty acid esterification under these conditions leads to a form of fatty liver characterized by small-droplet fat deposition allergy job market purchase clarinex 5mg, associated in severe cases with liver failure and hypoglycemia allergy shots 4 year old discount clarinex 5mg mastercard. The liver is the major source of endogenously synthesized cholesterol (approximately 0. Together with cholesterol of dietary origin, this newly synthesized cholesterol enters a "metabolically active" hepatic cholesterol pool, from which is derived the cholesterol destined for secretion into bile or into plasma (in lipoproteins), for synthesis of liver cell membranes, and for conversion to bile acids. Bile acid synthesis accounts for the disposition of approximately half of the total daily turnover of cholesterol and, as such, is an important determinant of body cholesterol stores. Relative rates of secretion of bile acids, cholesterol, and phosphatidylcholine (lecithin) into bile are important factors in the pathogenesis of cholesterol gallstones (see Chapter 152), but the mechanism(s) by which the secretion of these substances is effected and controlled is incompletely understood. Hepatic secretion of lipoproteins and clearance of chylomicron remnants are reduced in chronic liver disease, in part reflecting the thickened subendothelial basement membrane that blocks passage of large particles to and from the plasma membrane. Plasma protein synthesis totals 30 to 60 g/day and accounts for over 80% of all hepatic protein synthesis. In all cases, however, synthesis and secretion are dependent on the integrity of many aspects of cell function, including the transcriptional mechanisms in the nucleus, the translational mechanisms in the rough endoplasmic reticulum, the availability of amino acids, and the secretory mechanisms in the Golgi apparatus. Despite these common features, individual proteins are affected differently in liver disease. This variability may result from several factors such as the availability of an essential nutritional component. In addition, the kinetics of synthesis and turnover of a particular protein are major determinants of the response of its plasma concentration to acute liver injury. For these reasons, although liver disease generally tends to depress the plasma concentration of proteins of hepatic origin, plasma concentrations of such proteins may not accurately reflect the severity of the liver disease in a given patient. Interpretation of the prothrombin time, partial thromboplastin time, and serum albumin concentrations are useful in the evaluation of liver disease (see Chapter 147). Amino acids, in addition to their obvious importance in protein synthesis, also participate in other reactions in the liver. Of special significance is the role of certain amino acids as precursors for gluconeogenesis. Amino acids may undergo transamination, in which the alpha-amino group is transferred to an alpha-keto group, as in the alanine aminotransferase-mediated deamination of alanine to pyruvate; the resulting transfer of the amino group to alpha-ketoglutarate converts this acceptor to glutamate. In this case, an alpha-ketoacid is formed as the amino group is converted to ammonium ion and, ultimately, to urea (see later). The liver synthesizes all of the non-essential amino acids from their corresponding alpha-ketoacids. Severe liver disease is commonly associated with protein-calorie malnutrition, with relative plasma deficiency of branched-chain amino acids (leucine, isoleucine, and valine), and with accumulation of aromatic amino acids (phenylalanine and tyrosine). The reactions potentially involved are numerous and, in many instances, involve the cytochrome P-450-dependent microsomal mixed function oxidase system. In addition to the basic principles of drug disposition (see Chapter 26), several aspects warrant special emphasis in the context of liver function and disease. First, although biotransformation of an endogenous or exogenous substance may inactivate it or render it more suitable for urinary or biliary excretion, there are many examples of compounds that are rendered toxic by this process. A number of clinically significant hepatotoxins are activated in this way, and some "idiosyncratic" drug reactions may reflect individual differences in drug metabolism rather than an immunologic response (see Chapter 148). Second, diseases of the liver may seriously impair the biotransformation of exogenous substances, thereby resulting in an increased sensitivity to certain drugs. Finally, one substance may significantly influence the hepatic biotransformation of another. Examples of this particular form of drug-drug interaction include the well-recognized induction of the microsomal drug-metabolizing system by prior administration of phenobarbital and its inhibition by various toxins. A particularly important hepatic detoxification pathway converts ammonium ion to urea through the Krebs-Henseleit urea cycle, in which ornithine, citrulline, argininosuccinate, and arginine are intermediates and which involves both mitochondrial and cytosolic components. Ammonium ion is produced in abundance in the intestinal tract, especially the colon, by the bacterial degradation of luminal proteins and amino acids and of endogenous urea, 25% of the daily production of which diffuses into the intestinal lumen. Hepatic encephalopathy, which in part reflects the failure of this important detoxification process (and of analogous pathways for other endogenous and gut-derived toxins), may occur with either loss of functional liver cell mass or direct entry of portal blood into the peripheral circulation through spontaneous or surgically created portosystemic shunts (see Chapter 154). Lipoprotein abnormalities are common in liver disease and may predispose to vascular disease. Kondrup J, Nielsen K, Juul A: Effect of long-term refeeding on protein metabolism in patients with cirrhosis of the liver.
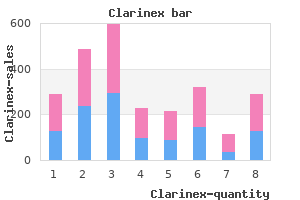
This is a prospective study demonstrating that melphalan-prednisone was superior to colchicine in 220 patients with primary amyloidosis allergy shots yes or no cheap clarinex 5 mg visa. Only 2 of the 25 patients with extramedullary plasmacytomas had development of multiple myeloma allergy symptoms during period safe 5 mg clarinex. Brenner Hematopoietic stem cell transplantation derives its feasibility from the biologic properties of these cells allergy shots sinusitis buy 5mg clarinex with amex. Even in small numbers (<106 /kg) allergy medicine holistic cheap clarinex 5mg overnight delivery, infused hematopoietic stem cells can completely and permanently repopulate a host with every marrow-derived lineage, including erythrocytes, myelocytes, monocytes, platelets, and T and B lymphocytes. Consequently, stem cell transplantation can treat defects arising in any of these lineages, and it can also be used to rescue patients from marrow aplasia arising from primary marrow disease or from the intensive cytotoxic chemotherapy that is used to treat malignancy. More recently, stem cell transplantation has been used to equip patients with genetically modified cells intended to combat several different inherited or acquired disorders and may also be valuable for mesenchymal cell disorders such as osteogenesis imperfecta (Table 182-1). The two types of stem cell transplantation are autologous, in which the patient is the cell donor, and allogeneic, in which the stem cells are derived from a separate individual. The morbidity of allogeneic stem cell transplantation increases as major and minor histocompatibility differences between the donor and patient increase. This increased morbidity largely results from alloreactivity, the recognition of self/non-self by donor and patient T lymphocytes. Dose intensification is limited by damage to normal organs, among the most sensitive of which is the bone marrow. One way of overcoming this limitation is to harvest and freeze hematopoietic stem cells from patients who have received conventional levels of therapy. This material is then infused to produce hematologic rescue following doses of chemotherapy/radiotherapy that would otherwise be lethal from marrow ablation. Because autologous transplants are not alloreactive, the procedure has a lower treatment-related morbidity and mortality than seen with allografting. However, the lack of an alloreactive "graft-versus-tumor" effect may explain why autografting generally has a higher risk of tumor relapse than allografting does. Relapse may also be associated with contamination of the graft with tumorigenic cells if these cells survive the conventional levels of chemotherapy that were given before stem cell harvest. Efforts to remove these cells by treating marrow with physical, pharmaceutical, or immunologic techniques are of uncertain benefit and may retard engraftment. Autografting is currently in wide clinical practice as treatment of a variety of hematologic and solid malignancies, including lymphoma and breast cancer. Unfortunately, there has been a disappointing lack of randomized studies to confirm that the approach genuinely increases patient survival in comparison to conventional chemotherapy/radiotherapy. Hence the usefulness of autologous transplantation in many malignant diseases remains uncertain. More recently, autologous transplantation has been used as a means of introducing genetically modified cells to treat inherited or 988 acquired disorders of hematopoietic cells. This approach is of great promise but is limited by the inefficiency of current gene transfer technologies. The value of autologous transplantation as treatment of severe autoimmune disorders is also under investigation. This approach is based on animal models in which it has been shown that "resetting" the immune system in this way may produce a long-term cure. For most non-malignant indications, allogeneic stem cell transplantation is the only current option. Under general anesthetic, marrow is removed though needle punctures made in the iliac crest. Sufficient marrow is removed to ensure engraftment (>1 Ч 108 nucleated cells per kilogram for autografting or >2 Ч 108 nucleated cells per kilogram for allografting); in adults, this number of cells usually translates to a volume between 0. Serious complications of this procedure are rare, although bruising and pain at aspiration sites are common. Infrequent but serious sequelae include the complications of anesthesia, as well as infection or cardiorespiratory instability. No general anesthetic or hospital stay is required, and the procedure can be performed by technical rather than medical staff. These characteristics not only reduce both the costs of the procedure and the accompanying morbidity but may also increase overall patient survival after autologous transplantation. However, some patients-especially those who have received extensive prior chemotherapy-may fail to mobilize and may then require marrow harvest in addition. However, locating and counseling prospective donors, performing phenotypic and molecular tissue typing, and harvesting the marrow require an average of 120 days, a delay that may doom a seriously ill patient.
Two careful discussions of professionalism in medicine and how it is a critical part of the health care system allergy testing kent cheap 5 mg clarinex. Singer Mark Siegler Clinical ethics is a practical discipline that contributes to improvement in patient care allergy shots weight loss buy clarinex 5 mg overnight delivery. It focuses on the central importance of patient preferences and choices in the patient-physician relationship and on the moral obligations of physicians allergy forecast league city buy 5 mg clarinex amex, such as the need for honesty allergy shots london cheap clarinex 5 mg on-line, competence, compassion, and respect for the patient. Clinical ethics teaches physicians about a wide range of specifically ethical issues-informed consent, truth telling, end-of-life decisions, advance directives, and increasing third-party constraints on the autonomy of both patients and physicians. Although in theory these issues have been resolved, in practice they continue to vex conscientious physicians. The most clinically important ethical issues that arise frequently in the practice of internal medicine include decision making by competent patients, substitute decision making (including advance directives) for incompetent patients, end-of-life decisions, futility, and clinical-ethical concerns in an era of cost containment and health care reform. Most clinical decisions are now reached by a process of shared decision making in which physicians provide information and guidance that allow competent adult patients to base decisions on their own personal preferences, values, and goals. Competent adult patients have an ethical and legal right to accept or refuse medical care recommended by physicians, including life-sustaining treatments. The clinical-ethical process of shared decision making is mirrored by the legal doctrine of informed consent. Informed consent is defined as voluntary acceptance by a competent patient of a plan for medical care after the physician adequately discloses the proposed plan, its risks and benefits, and alternative approaches. The informed consent process applies not only to invasive surgical procedures but to every clinical decision as well. If the patient has decision-making capacity (see later), the physician should seek consent from the patient; if the patient lacks decision-making capacity, the physician should seek consent from the appropriate substitute decision maker. The best way for young physicians to learn how to obtain informed consent from patients is by observing a clinician who is recognized for skill in negotiating the consent process. Perhaps the clearest legal statement of this right was enunciated in 1914 by Justice Cardozo: "Every human being of adult years and sound mind has the right to determine what shall be done with his body. In the 1980s, a presidential commission clearly stated that respect for patient preferences should be the basis of public policy in medical ethics. Moreover, evidence from clinical research indicates that patients who participate in their own health care decisions are more likely to implement the shared decision, express greater satisfaction with their physician, and most importantly, have improved functional outcomes in several chronic diseases. For the purposes of informed consent, disclosure must include proposed diagnostic tests and treatments, their risks and benefits, and possible alternative approaches. For example, physicians would be expected to inform patients about risks that are either highly likely to occur or less likely but very serious when they do occur. Another aspect of disclosure separate from the need to obtain informed consent involves telling patients the truth about unfavorable diagnoses, such as metastatic cancer, and their prognoses. In the United States, the current medical standard is to be honest with patients and not to conceal bad news. Decision-making capacity, a clinical concept, is the ability to understand relevant information and appreciate the consequences of a decision. Patients who have been determined to have decision-making capacity should make their own health care decisions, based on the principle of autonomy, whereas patients determined to lack it should be protected from making bad and sometimes irreversible decisions, based on the principle of beneficence. Decision-making capacity is a dynamic state and may change quickly, as when a patient is admitted stuporous, hypotensive, and with sepsis and lacks this capacity but, 12 hours later, after appropriate treatment, is sitting in bed, conversing normally, and has regained it. For example, patients with substantial cognitive impairment may retain decision-making capacity to decide whether they wish to accept a recommended elective cholecystectomy. Unfortunately, no valid and widely accepted clinical measures are available to assess decision-making capacity. Physicians should assess this capacity by asking patients whether they understand and appreciate their medical problem and the risks and benefits of the proposed treatment and why they have chosen to accept or reject it. When doubt exists, consultation with a psychiatrist or neurologist may be helpful. Disagreements about decision-making capacity are often brought to the attention of hospital attorneys, ethics committees, or ethics consultants. Often, however, the tempo of clinical circumstances may require physicians to make decisions by relying on clinical judgment and assistance from consultants to reach the best and most ethical determination. In practice, however, patients who lack decision-making capacity cannot exercise this right.
Cheap clarinex 5mg with mastercard. Allergy Symptoms & Treatments : How to Cure Dust Allergies.
© 2020 Vista Ridge Academy | Powered by Blue Note Web Design




