"Discount 30g lidocaine free shipping, symptoms of a stranger".
By: V. Cruz, MD
Professor, University of Hawaii at Manoa John A. Burns School of Medicine
However treatment hyponatremia buy lidocaine 30g line, these motor movements medications breastfeeding purchase 30g lidocaine with amex, especially early in coma medications used for migraines order lidocaine 30g amex, are most frequently fragments of abnormal medicine to calm nerves discount lidocaine 30g otc, asymmetrical flexion and extension in the arms rather than the complete decorticate and decerebrate postures illustrated in the figure. A small amount of asymmetrical flexion or extension of the arms in response to painful stimulus carries the same implications as the full-blown postures. Metabolic lesions do not compromise the brain in a progressive level-by-level manner as do hemispheric masses and rarely produce the asymmetrical motor signs typical of masses. If the pupils constrict to a bright light, the midbrain is intact, and if they do not, the midbrain has been compromised. In mass lesions, the loss of pupillary reactivity from a hemispheric mass is asymmetrical, with the pupil homolateral to the mass losing reactivity before its contralateral fellow. A midbrain pupil may be large and unreactive if the descending sympathetic pathways in the brain stem have not been compromised but are more commonly at midposition (5 mm), reflecting both parasympathetic (third nerve) and sympathetic (brain stem) injury. In metabolic coma one feature is central to the examination: Pupillary reactivity is present. Early and late diencephalic levels are levels of dysfunction just above (early) and just below (late) the thalamus. The medial longitudinal fasciculus traverses the dorsal pons to connect with the third cranial nerve (moving the eye medially). With metabolic coma of non-drug-induced origin such as organ system failure or electrolytic or osmolar disorders, reflex eye movements are preserved. Ocular bobbing (spontaneous symmetrical or asymmetrical rhythmic vertical ocular oscillations) may be seen. A number of syndromes of multifocal vascular disease are characterized by diffuse brain dysfunction that appears to be a metabolic encephalopathy. However, prolonged alteration in consciousness after an unwitnessed seizure may produce diagnostic confusion. Such prolonged post-ictal states follow seizures affecting an acutely or chronically impaired brain. Locked-in syndrome patients are those in whom a lesion (usually hemorrhage or an infarct) transects the brain stem at a point below the reticular formation (therefore sparing consciousness) but above the ventilatory nuclei of the medulla (therefore, precluding death). Such patients are awake, with eye opening and sleep-wake cycles, but have transection of the descending pathways through the brain stem necessary for volitional vocalization or limb movement. Voluntary eye movement, especially vertical, is preserved, and patients open and close their eyes or produce appropriate numbers of blinking movements in answer to questions. Magnetic stimulation of motor cortex producing motor evoked potentials may be an additional positive prognostic feature. Ice water caloric testing will either arouse the patient because of the discomfort produced or induce cortically mediated nystagmus rather than the tonic deviation typical of coma. The slow conjugate roving eye movements of metabolic coma cannot be imitated and, therefore, exclude psychogenic unresponsiveness. In addition, the slow, often asymmetrical, and incomplete eye closure that follows passive eyelid opening of a comatose patient cannot be feigned. Data from Edgren E et al: Assessment of neurological prognosis in comatose survivors of cardiac arrest. Motor: No response (one), reflex extension (two), reflex flexion (three), complex flexion (four), localizes pain (five). Pupils: No reactivity (zero), unilateral reactivity (one), bilateral reactivity (two). Brisk, small-amplitude, mainly vertical eye movements are seen in patients with ischemia-induced electrographic status epilepticus and are predictive of a fatal outcome. In cardiac arrest patients without the complicating issue of seizures, return of pupillary reactivity and purposeful motor movements within the first 72 hours is highly correlated with a favorable outcome (Table 444-2). The outcome after traumatic head injury is more difficult to assess and includes an additional prognostic factor: age. Young patients (less than 20 years) are over three times more likely to survive than those above age 60.
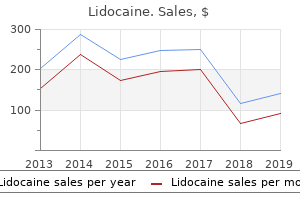
Flat or inverted T waves suggest a low potassium level symptoms yellow fever 30g lidocaine with mastercard, and peaked T waves suggest high intracellular potassium medications xyzal 30g lidocaine visa. The intracellular potassium deficit in renal tubular cells further promotes potassium loss by the kidneys medicine zebra 30g lidocaine free shipping, and this abnormality does not correct immediately symptoms of diabetes generic 30g lidocaine fast delivery. Suppression of lipolysis by insulin reduces free fatty acid flux to the liver and ketogenesis. The remaining keto acids are oxidized, with subsequent regeneration of bicarbonate. The hyperventilatory drive of severe acidosis is uncomfortable, and severe acidosis has a negative inotropic effect and causes vasodilation. In addition, by causing a sudden left shift of the dissociation curve for oxyhemoglobin, bicarbonate may impair oxygen delivery to tissues. Although substantial phosphate depletion occurs with both diabetic ketoacidosis and 1279 non-ketotic hyperosmolar syndrome, the prophylactic use of phosphate in diabetic ketoacidosis has failed to show any significant benefit. Because the longer prodromal period associated with non-ketotic hyperosmolar syndrome may lead to more severe phosphate losses, they may need to be replaced as potassium phosphate together with magnesium. When severe hypovolemia or renal dysfunction is present, central venous pressure monitoring is indicated. Urinary catheterization is essential in unconscious or oliguric patients, and gastric decompression may be required to minimize the risk of aspiration. Table 242-8 outlines the principles of management of diabetic ketoacidosis and non-ketotic hyperosmolar syndrome. Alcoholic ketoacidosis may be confused with diabetic ketoacidosis, particularly when hyperglycemia is present. It is typically seen in people who have consumed large amounts of alcohol and then abstain from food or drink for an extended period. Hyperglycemia is probably limited because hepatic metabolism of alcohol leads to an increase in the ratio of reduced to non-reduced nicotinamide adenine dinucleotide, which inhibits gluconeogenesis despite insulin deficiency. Alcoholic ketoacidosis is rapidly reversed by the intravenous administration of fluids and glucose; insulin is rarely needed, except in diabetic persons. This problem tends to occur in elderly diabetics with impaired renal function and is more common with the longer-acting sulfonylureas. Nevertheless, hypoglycemia may provoke seizures, accidental injury, and a catecholamine response that can induce arrhythmias or cardiac ischemia in patients with underlying cardiac disease. Hypoglycemia is thought to account for 3 to 4% of deaths in insulin-treated diabetic patients. In normal persons, hypoglycemia provokes a response that returns blood glucose to normal. If glucose efflux from the circulation exceeds exogenous and endogenous influx, hypoglycemia results. The rise in glucose production is initiated by the release of glucagon, as well as epinephrine, in conjunction with a fall in endogenous insulin release and, at the outset, probably reflects mainly the stimulation of hepatic glycogenolysis. In addition, these patients for unclear reasons have attenuated or absent glucagon secretion during hypoglycemia, although glucagon responses to other stimuli persist. Unfortunately, nearly half of type 1 patients with disease for over 10 years also undergo a stimulus-specific diminution in their epinephrine response to hypoglycemia that increases its risk. Symptoms and signs of glucose deficiency in the central nervous system, termed neuroglycopenia, may be non-specific. Loss of awareness of symptoms is more likely to be found in patients with long disease duration and is associated with an absent or impaired sympathoadrenal response. The duration of diabetes, however, is not the only factor responsible for impaired adrenergic and symptomatic responses to hypoglycemia. Similar phenomena may also occur when patients are switched to intensive insulin regimens. The mechanism underlying the changes is the increased appearance of iatrogenic hypoglycemia during intensified insulin therapy; it has been shown that brief periods of antecedent hypoglycemia suppress counterregulatory hormone responses and symptoms during subsequent hypoglycemia for several days. Thus hyperglycemia induces widespread modifications in cellular and structural proteins that may contribute to long-term complications. Other potential biochemical mechanism s through which hyperglycemia could impair cell function include (1) the polyol pathway through which non-phosphorylated glucose is reduced to sorbitol by aldose reductase, which in turn leads to changes in the intracellular oxidation-reduction state, and (2) increased diacylglycerol production with subsequent activation of specific isoforms of protein kinase C. Beneficial effects of aldose reductase inhibitors and specific protein kinase C inhibitors have been demonstrated in animal models of diabetes; however, such effects have not been convincingly shown in patients. Hemodynamic changes in the microcirculation may also contribute to microangiopathy.
After 6 to 8 weeks medicine youtube 30g lidocaine with visa, the clinical course becomes more static as fibrosis symptoms 12 dpo discount lidocaine 30g with mastercard, hyperinflation medications education plans order 30g lidocaine free shipping, and pulmonary edema come to dominate the clinical picture schedule 8 medications list lidocaine 30g line. Increased airway smooth muscle is present and tracheobronchomalacia may become apparent as episodes of acute airway collapse with severe hypoxemia. This phase evolves over 3 to 9 months, during which time growth and remodeling of lung parenchyma and the pulmonary vascular bed is associated with gradual improvement in pulmonary function and heart-lung interaction. Such infants may remain ventilator-dependent for several weeks and then improve progressively. During this Guidelines for Acute Care of the Neonate, Edition 26, 201819 25 Section 2-Respiratory Care Section of Neonatology, Department of Pediatrics, Baylor College of Medicine In most infants, extubation can be attempted from stable ventilator settings once oxygen requirement gradually falls to consistently 40% or less, infant is anabolic (as demonstrated by weight and linear growth trends), and the infant is beyond the phase characterized by wide swings in oxygen saturations described earlier. However, the infant remains vulnerable to pulmonary edema and reactivation of the inflammatory process within the lungs with deterioration in function. Most patients continue to exhibit significant pulmonary hypertension and attempts to wean oxygen or positive pressure support too rapidly may precipitate acute cor pulmonale. Serum urea nitrogen, calcium, phosphorus, and alkaline phosphatase values should be determined periodically. Nutritional and growth parameters should be reviewed frequently with a pediatric nutritionist. Chronic Mechanical Ventilation: Minimal Impact Respiratory Support Long-term monitoring Over the first year of life, active inflammation diminishes and the process of repair and remodeling of the lung becomes more orderly. Lung growth and remodeling slowly progresses, allowing improving pulmonary function and decreasing need for positive pressure support. However, lung mechanics remain quite abnormal; hyperinflation, fibrosis, and cysts may remain visible on radiographs. Many of these infants exhibit persistent evidence of fixed airway obstruction and some have episodes of typical asthma. A more detailed description of chronic mechanical ventilation has been described in a previous section. However, oxygen also may exacerbate lung injury and risk of retinopathy in preterm infants. The need for supplemental O2 often extends well beyond the period of positive pressure ventilator support. Prevention of cor pulmonale Nutritional Support Complete nutrient intake must be provided despite significant fluid restriction. Although adequate calories may be provided using fat or carbohydrate additives, the intake of protein, minerals, and micronutrients will be insufficient unless they, too, are supplemented. The balance between fluid restriction, adequate growth, and stability of lung function requires frequent reassessment. In preterm infants, modest fluid restriction (150 ml/kg/day) and proper long-term nutrition often can be achieved using fortified human milk or one of the commercial mineral-enhanced premature formulas. These provide good quality protein intake, trace nutrients, and increased calcium and phosphorus supplements to optimize bone mineral uptake. When the infant reaches term, a standard or mineral- and protein-enriched transitional formula may be substituted. Severe impairment of lung mechanics may necessitate restricting fluids to 110-130 26 the care environment is critical for chronically ventilatordependent infants. The adverse impact of the intensive care environment upon development must be blunted during a long period of hospitalization. A respiratory strategy that de-emphasizes day-to-day-variation and addresses the long-time constant physiology of obstructive lung disease will minimize air hunger, ventilator dyssynchrony, and gas trapping, making the need for sedatives and paralytics less likely. Some patients have associated neurologic dysfunction, hearing deficits, or feeding disorders, and the resources to manage these problems must be integrated into weekly schedules. Cardiac catheterization should be considered prior to initiating long-term therapy to assess severity of disease and potential contributing factors, such as left ventricular diastolic dysfunction, anatomic shunts, pulmonary vein stenosis, and systemic collaterals If pulmonary hypertension present: a. Evaluate and treat respiratory disease, including assessing for hypoxemia, aspiration, and structural disease b. Developmental assessment should begin during the hospital stay and continue as part of long-term follow-up after discharge. Specific attention to oral-motor dysfunction and feeding disorders may be necessary. Monitoring: Cardiac catheterization or serial echocardiography is recommended to monitor response to therapy.
Lidocaine 30g online. Getting Anxiety Symptoms Out of Nowhere? (I DID TOO!).
Some patients with thalamic hemorrhages lose consciousness early in the clinical course treatment tennis elbow 30g lidocaine for sale, but those who are awake often experience contralateral hemiparesis medicine 93832 cheap lidocaine 30g online, sensory changes medicine 50 years ago cheap lidocaine 30g without a prescription, and homonymous hemianopsia (the last often clearing quickly) medicine qd discount lidocaine 30g otc. Because cerebellar hemorrhage initially spares the brain stem, consciousness is usually preserved in the early stages. Occipital headache is usually the first symptom, followed by unsteady gait, clumsiness, nausea, and vomiting, which may be severe and repetitive. Prompt recognition and treatment of cerebellar hemorrhage by this stage can be life saving. The clinical presentation depends on the actual location of the hemorrhage, but there are some common features. Most patients are elderly; headache, nausea, and vomiting probably occur with about the same frequency but less intensity as in deep, hypertensive hemorrhages. Coma and seizures are less common, possibly because the bulk of the hemorrhage is comparatively small and located in subcortical white matter. Cerebral angiography is seldom used to evaluate acute hemorrhages, except those attributed to mycotic aneurysms being evaluated for surgical intervention. Incipient herniation is initially treated with hyperventilation (which takes advantage of the vasoconstricting effect of hypocapnia; see Chapter 469) and osmotic agents. Corticosteroids have not been effective in treating brain edema from cerebral hemorrhage, and since they carry added risks. With the cerebellum, lateral ventricular shunting appears to produce results as good as or better (fewer neurologic residua) than surgical removal of hematomas, although lesions more than 3 cm in diameter that continue to compress the brain stem after the shunt is placed occasionally benefit from evacuation. As with ischemic stroke, recent studies show that about 20% of patients who survive hemorrhage require institutionalization; in contrast to ischemic stroke, however, most of the remaining survivors of hemorrhage achieve a good status or complete recovery. Age and large hemorrhage size are associated with a worse prognosis, and prognosis after extensive brain stem hemorrhage is guarded. At present, there is no way to control the risk of bleeding from amyloid angiopathy. One theory, largely discounted, was based on observed retinal vasospasm and suggested that similar intracerebral vasospasm caused focal ischemia and resultant neurologic dysfunction. Resulting local and diffuse edema is postulated to cause the focal and diffuse neurologic changes. Hypercapnia, by dilating cerebral blood vessels, can exacerbate the effects of hypertensive encephalopathy, and seizures also are associated with further increases in cerebral blood flow and capillary pressure. Both should be avoided by controlled ventilation, when required, with anticonvulsants such as intravenous diazepam, 10 to 20 mg given slowly in repeated doses as needed to control seizures, and followed by phenytoin or carbamazepine. The neurologic manifestations of viral infections are also diverse, extending from the acute febrile encephalitides to chronic progressive neurodegenerative disorders. A neurotropic virus is one that infects cells within the nervous system, and a neurovirulent virus causes clinically recognizable neurologic symptoms. Most viral infections are asymptomatic, and nervous system involvement is an uncommon complication of a relatively common systemic infection. For example, the polioviruses cause enteric infections in which replication in the gut and fecal-oral transmission determine the essential survival and transmission of the organism; extension of infection to anterior horn cells of the spinal cord devastates the host but does not contribute to the "life cycle" of the virus. The virus may enter through the choroid plexus and spread through cerebrospinal fluid pathways or, alternatively, invade the brain by crossing the blood-brain barrier. Within the nervous system, some viruses do not discriminate among neurons and glial or endothelial cells, whereas others infect selective targets. Productive infection is characterized by a full replication cycle with production of virions. If there is a prolonged release of low level of virions without cell death, it is termed persistent infection. Transforming infection causes increased and characteristically abnormal cell proliferation and thereby oncogenic transformation of the cells, usually in the absence of virus replication. Neural injury and dysfunction accompanying viral infections may be due to direct infection of the cells. The relative importance of these factors in individual infections depends on both the interactions of the invading organism with the cells it infects and the profile of host cell responses that it elicits. Diagnostic approaches to viral diseases depend on the clinical setting and specific agents involved.
© 2020 Vista Ridge Academy | Powered by Blue Note Web Design




